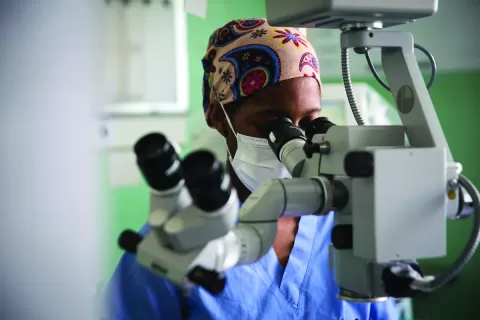
Evidence Based Care
155
Education scholarship awarded over the years
30
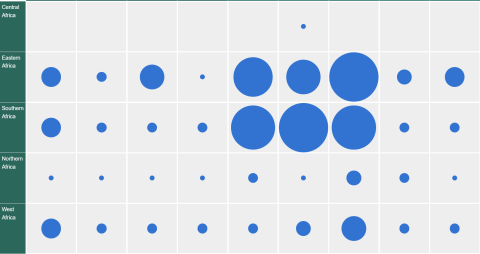
Countries Supported to develop Palliative Care Services
275
Small grants awarded towards the support of palliative care service delivery
985
Children receiving Palliative care (Small Grants)
23581
Adults receiving palliative care (Small grants scheme)
20
African Ministers of Health meetings on palliative care convened
173
Peer reviewed palliative care publications
86
Partnerships developed across geographical regions
Discover more from our Evidence Section.
Latest Announcements
- Added:
- Added:
- Added:
- Added:
Stories from APCA
Explore the latest stories, news & articles from APCA
Every year, millions of people in Africa suffer from life-threatening and chronic illnesses, and the majority of them do not have access to quality palliative care
Donations, however large or small, are vital to African Palliative Care Association APCA’s ongoing work. Consider making a personal or corporate donation today to enable us to improve the quality of life for people with life-threatening illnesses, their families and their carers in Africa.